Urinary incontinence - retropubic suspension
Retropubic suspension is surgery to help control stress incontinence. This is urine leakage that happens when you laugh, cough, sneeze, lift things, or exercise. The surgery helps close your urethra and bladder neck. The urethra is the tube that carries urine from the bladder to the outside. The bladder neck is the part of the bladder that connects to the urethra.
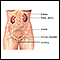
Stress incontinence
Stress urinary incontinence occurs when your bladder leaks urine during physical activity or exertion. It may happen when you cough, sneeze, lift so...
Description
You receive either general anesthesia or spinal anesthesia before the surgery starts.
General anesthesia
General anesthesia is treatment with certain medicines that puts you into a deep sleep-like state so you do not feel pain during surgery. After you ...
Read Article Now Book Mark Article- With general anesthesia, you are asleep and feel no pain.
- With spinal anesthesia, you are awake but numb from the waist down and feel no pain.
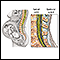
Spinal anesthesia
Spinal and epidural anesthesia are procedures that deliver medicines that numb parts of your body to block pain. They are given through shots in or ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
A catheter (tube) is placed in your bladder to drain urine from your bladder.
There are 2 ways to do retropubic suspension: open surgery or laparoscopic surgery. Either way, surgery may take up to 2 hours.
During open surgery:
- A surgical cut (incision) is made on the lower part of your belly.
- Through this cut the bladder is located. The surgeon sews (sutures) the bladder neck, part of the wall of the vagina, and the urethra to the bones and ligaments in your pelvis.
- This lifts the bladder and urethra so they can close better.
During laparoscopic surgery, the surgeon makes a smaller cut in your belly. A tube-like device that allows the doctor to see your organs (laparoscope) is put into your belly through this cut. The surgeon sutures the bladder neck, part of the wall of the vagina, and the urethra to the bones and ligaments in the pelvis.
Why the Procedure Is Performed
This procedure is done to treat stress incontinence.
Before discussing surgery, your surgeon will have you try bladder retraining, Kegel exercises, medicines, or other options. If you tried these and are still having problems with urine leakage, surgery may be your best option.
Risks
Risks for any surgery are:
-
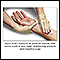
Bleeding
Bleeding
Bleeding is the loss of blood. Bleeding may be:Inside the body (internal)Outside the body (external)Bleeding may occur:Inside the body when blood le...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
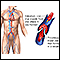
Blood clots in the legs that may travel to the lungs
Blood clots
Blood clots are clumps that occur when blood hardens from a liquid to a solid. A blood clot that forms inside one of your veins or arteries is calle...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
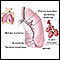
Breathing problems
Breathing problems
Breathing difficulty may involve:Difficult breathing Uncomfortable breathingFeeling like you are not getting enough air
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Infection in the surgical cut, or opening of the cut
- Other infection
Risks for this surgery are:
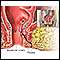
- Abnormal passage (fistula) between the vagina and the skin
Fistula
A fistula is an abnormal connection between two body parts, such as an organ or blood vessel and another structure. Fistulas are usually the result ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Damage to the urethra, bladder, or vagina
Damage to the urethra, bladder
Traumatic injury of the bladder and urethra involves damage caused by an outside force.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Irritable bladder, causing the need to urinate more often
- More difficulty emptying your bladder, or the need to use a catheter
- Worsening of urine leakage
Before the Procedure
Tell your health care provider and surgeon what medicines you are taking. These include medicines, supplements, or herbs you bought without a prescription.
Tell your surgeon or nurse if:
- You are or could be pregnant
- You are taking any medicines, including medicines, supplements, or herbs you bought without a prescription
- You have been drinking a lot of alcohol, more than 1 or 2 drinks a day
Planning for your surgery:
- If you have diabetes, heart disease, or other medical conditions, your surgeon may ask you to see the provider who treats you for these conditions.
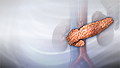
Diabetes
Diabetes is a long-term (chronic) disease in which the body cannot regulate the amount of sugar in the blood.
 ImageRead Article Now Book Mark Article
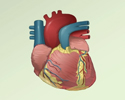
ImageRead Article Now Book Mark ArticleHeart disease
Coronary heart disease is a narrowing of the blood vessels that supply blood and oxygen to the heart. Coronary heart disease (CHD) is also called co...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - If you smoke, it's important to cut back or quit. Smoking can slow healing and increase the risk for blood clots. Ask your provider for help quitting smoking.
Smoking can slow healing and increase t...
Quitting smoking and other nicotine products, including e-cigarettes, before surgery can improve your recovery and outcome after surgery. Most people...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleQuitting smoking
There are many ways to quit smoking. There are also resources to help you. Family members, friends, and co-workers may be supportive. But to be su...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - If needed, prepare your home to make it easier to recover after surgery.
Prepare your home
Getting your home ready after you have been in the hospital often requires some preparation. Set up your home to make your life easier and safer when...
Read Article Now Book Mark Article - Ask your surgeon if you need to arrange to have someone drive you home after your surgery.
During the week before your surgery:
- You may be asked to temporarily stop taking medicines that keep your blood from clotting. These medicines are called blood thinners. This includes over-the-counter medicines and supplements such as aspirin, ibuprofen (Advil, Motrin), naproxen (Aleve, Naprosyn), and vitamin E. Many prescription medicines are also blood thinners.
- Ask your surgeon which medicines you should still take on the day of surgery.
- Let your surgeon know about any illness you may have before your surgery. This includes COVID-19, a cold, flu, fever, herpes breakout, or other illness. If you do get sick, your surgery may need to be postponed.
COVID-19
Coronavirus disease 2019 (COVID-19) is a respiratory illness that causes fever, coughing, and shortness of breath, but many other symptoms can occur....
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleCold
The common cold most often causes a runny nose, nasal congestion, and sneezing. You may also have a sore throat, cough, headache, or other symptoms....
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleFlu
The flu (influenza) is a viral respiratory illness that causes fever, chills, runny nose, body aches, and cough. It spreads easily from person to pe...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
On the day of surgery:
- Follow instructions about when to stop eating and drinking.
- Take the medicines your surgeon told you to take with a small sip of water.
- Follow instructions on when to arrive at the hospital. Be sure to arrive on time.
After the Procedure
You will likely have a catheter in your urethra or in your abdomen above your pubic bone (suprapubic catheter). The catheter is used to drain urine from the bladder. You may go home with the catheter still in place. Or, you may need to perform intermittent catheterization. This is a procedure in which you use a catheter only when you need to urinate. You will be taught how to do this before you leave the hospital.
Catheter
A urinary catheter is a tube placed in the body to drain and collect urine from the bladder.
You may have gauze packing in the vagina after surgery to help stop bleeding. It is usually removed a few hours after surgery.
You may leave the hospital on the same day as surgery. Or, you may stay for 2 or 3 days after this surgery.
Follow instructions about how to care for yourself after you go home. Keep all follow-up appointments.
Care for yourself after you go home
Getting your home ready after you have been in the hospital often requires some preparation. Set up your home to make your life easier and safer when...
Read Article Now Book Mark ArticleOutlook (Prognosis)
Urinary leakage decreases for most women who have this surgery. But you may still have some leakage. This may be because other problems are causing your urinary incontinence. Over time, some or all of the leakage may come back.
Reviewed By
Kelly L. Stratton, MD, FACS, Associate Professor, Department of Urology, University of Oklahoma Health Sciences Center, Oklahoma City, OK. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
Hartigan SM, Chapple CR, Dmochowski RR. Retropubic suspension surgery for incontinence in women. In: Partin AW, Dmochowski RR, Kavoussi LR, Peters CA, eds. Campbell-Walsh-Wein Urology. 12th ed. Philadelphia, PA: Elsevier; 2021:chap 123.
Kobashi KC, Vasavada S, Bloschichak A, et al. Updates to surgical treatment of female stress urinary incontinence (SUI): AUA/SUFU Guideline (2023). J Urol. 2023;209(6):1091-1098. PMID: 37096580 pubmed.ncbi.nlm.nih.gov/37096580/.
Lentz GM, Miller JL. Lower urinary tract function and disorders: physiology of micturition, voiding dysfunction, urinary incontinence, urinary tract infections, and painful bladder syndrome. In: Gershenson DM, Lentz GM, Valea FA, Lobo RA, eds. Comprehensive Gynecology. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 21.
Disclaimer


 All rights reserved.
All rights reserved.